Table of Contents
The enteric nervous system (ENS) is also known as the “second brain” because of its ability to function independently from the central nervous system (CNS). It is a complex network of neurons that control the functions of the gastrointestinal (GI) tract, including the movement of food through the digestive tract, the release of enzymes and hormones, and the regulation of blood flow to the gut independently of CNS although CNS can influence the activity of ENS.
The ENS is made up of two main components: the myenteric plexus and the submucosal plexus which differ in their location and functions. The enteric nervous system is quite important in maintaining the normal functioning of GIT and overall health as it performs several crucial functions for optimum health.
Anatomy of the enteric nervous system
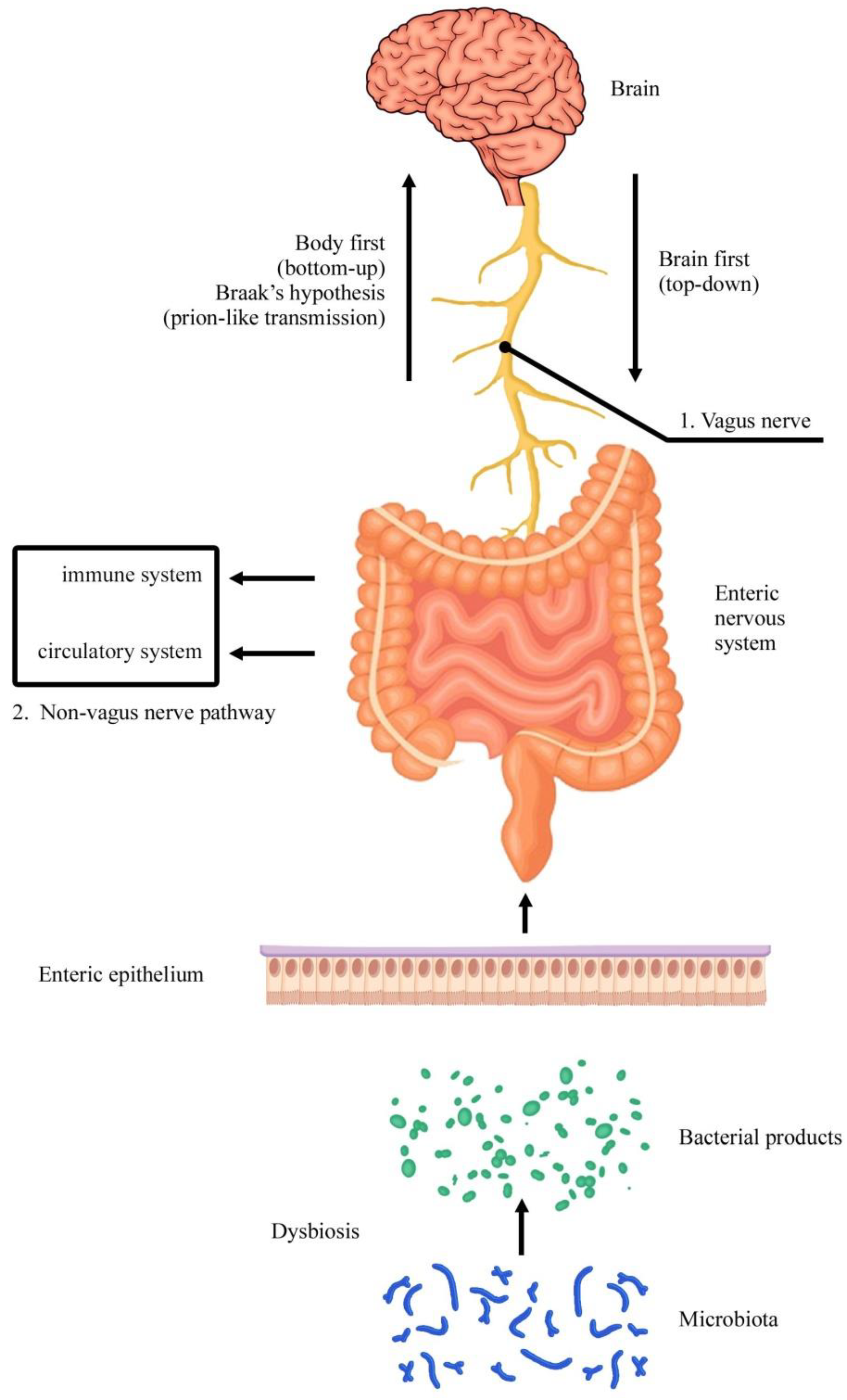
The gastrointestinal tract is a unique organ that is exposed to a large variety of physiochemical stimuli from the external world in the form of food we eat. As a result, the gastrointestinal tract has developed a rich coordinated pattern of movements controlled by ENS to ensure that there is appropriate mixing, digestion, and propulsion of the ingested contents. The oro-aboral transmission of intestinal contents is a result of adaptive locomotion as a result of complex interactions between the muscular and neuronal apparatus of GIT. The innermost layer of GIT is mucosa which contains specialized epithelial cells. The submucosa is located under the mucosa and contains nerves, large blood vessels, and connective tissue. Meissner’s plexus is located near the outer margin of the submucosa.
The muscular apparatus of the gastrointestinal tract is in the form of interconnected smooth muscle cells which are electrically linked to each other via gap junctions to function as large mechanical units. It has an inner circular and outer longitudinal layer separated by the myenteric plexus. The gastrointestinal tract has pacemaker cells called interstitial cells of Cajal which control the propulsive GIT movements. The outermost layer of GIT is formed by fats and epithelial cells.
The neuronal apparatus of the enteric nervous system comprises myenteric and Meissner’s plexuses which are composed of a large number of neurons that differ according to their location, shape, projections, connections, neurochemistry, and function. Like the central nervous system controlling sensory-motor functions, ENS also contains afferent neurons to detect stimuli, interneurons to process the information, and efferent neurons to produce the response. The neuronal network of ENS extends through the entire length of the gastrointestinal tract to ensure the proper functioning of GIT.
The myenteric plexus, also known as Auerbach’s plexus, is located between the inner and outer layers of the muscularis externa. The myenteric plexus is a collection of myelinated neurons and postganglionic autonomic cell bodies. The neurons in this plexus provide input to both layers of muscularis externa and control their rhythmic contractions for food propulsion. The plexus has sensory receptors to detect chemical or mechanical stimuli which are processed by interneurons of the enteric nervous system to produce the response. The myenteric plexus has rich interconnections with the brain stem through anterior and posterior vagal nerves. The submucosal plexus also known as Meissner’s plexus is a neuronal network in the submucosa concerned mainly with the secretions in GIT.

Enteric neurons
The enteric neurons include primary afferent neurons, excitatory circular muscle motor neurons, longitudinal muscle motor neurons, inhibitory circular muscle motor neurons, ascending interneurons, descending interneurons, secretomotor & vasomotor neurons, and intestinofugal neurons. Let’s discuss them individually:
Primary afferent neurons
Primary afferent neurons also known as enteric or intrinsic primary afferent neurons are present in both myenteric and Meissner’s plexuses. They respond to muscle stretch, tension in the mucosa, chemical stimuli in the lumen, or mucosal deformation. They make up about 30% of myenteric neurons and about 14% of the submucosal neurons and have distinct shapes. They all project to the villi and branch in the myenteric and mucosal ganglia. A small portion of these neurons also send projections to the aboral myenteric ganglia and receive slow synaptic input via tachykinins from primary afferent neurons to form reciprocally innervated circuits. Enteric afferent neurons make synapses with the ascending and descending interneurons and stimulate the excitatory or inhibitory motor neurons to circular or longitudinal muscles.
Excitatory circular muscle motor neurons
They are the final motor neurons of the circular smooth muscles of the intestine. They are innervated either via nicotinic stimulation or slow synaptic input from the local primary afferents. They are also stimulated by cholinergic ascending interneurons and descending interneurons. These neurons project to circular smooth muscles and form deep muscular plexus of dense nerve fibers. They release acetylcholine and tachykinins as neurotransmitters to stimulate smooth muscles either directly or through the interstitial cells in the deep muscular plexus.
Inhibitory circular muscle interneurons
They are innervated by fast nicotinic transmission from the primary afferent neurons and noncholinergic inputs from the descending afferents. They project to the circular muscles and are linked to the excitatory motor neurons in the deep muscular plexus. They inhibit circular muscles, either directly or indirectly, by releasing several neurotransmitters such as nitric oxide, ATP, pituitary activating cAMP peptide, and vasoactive intestinal peptides.
Longitudinal muscle motor neurons
These neurons control the contractility of longitudinal smooth muscles of GIT. They are innervated by enteric primary afferent neurons and ascending and descending interneurons.
Ascending interneurons
These neurons form a long ascending tract of interneurons. They receive fast nicotinic and slow synaptic innervation through the primary enteric afferent neurons. They form synapses with the excitatory circular muscle motor neurons via fast nicotine or noncholinergic transmission. They contain enzymes for the synthesis of neurotransmitters such as acetylcholine, opioids, and tachykinins.
Descending interneurons
Descending interneuron neurons differ from each other depending on their neurochemistry. Somatostatin and choline acetyltransferase containing descending interneurons receive input from the nonprimary afferents and form a long chain of interneurons synapsing with myenteric and Meissner’s plexuses. Serotonin interneurons project to the aboral myenteric and Meissner’s neurons but don’t cause inhibition. The dual linkage of these neurons to both myenteric and Meissner’s plexuses reflects the functional linkage between the motor, vasomotor, and secretory fibers.
Secretomotor & vasomotor fibers
Two classes of secretomotor fibers are found in the myenteric ganglia. One class uses acetylcholine as a neurotransmitter while the other uses vasoactive intestinal peptides. These neurons project to the mucosa of GIT. Neurons with similar neurochemistry, releasing acetylcholine and VIP, are present in submucosal ganglia in proportions of 32% and 42% respectively. Some VIP neurons from the submucosa project to the myenteric ganglia showing that there is a functional connection between motility and secretion. The submucosal VIP secretomotor neurons also receive inhibitory input from the sympathetic nervous system. The cholinergic neurons from the submucosa also project to the local blood vessels.
Intestinofugal neurons
These are a small group of cholinergic neurons projecting from the myenteric ganglia to the prevertebral ganglia.
Read more about the Functions of the Autonomic Nervous System
Neurotransmitters of the enteric nervous system
The enteric nervous system also contains a large number of neurotransmitters, which are chemical messengers that transmit signals between neurons. The most important neurotransmitters in the enteric nervous system are acetylcholine, substance P, tachykinins, serotonin, enkephalin, endorphins, nitric oxide, and vasoactive intestinal peptide. Acetylcholine acts on muscarinic receptors in the gut and increases the GIT motility and secretions, while substance P and serotonin regulate secretions and absorptions.
Enkephalin and endorphins are released by the intrinsic sensory neurons in the enteric nervous system and regulate the pain sensation in the GIT. Nitric oxide produced by the nitrergic neurons in GIT regulates the tone of smooth muscles and controls the blood flow in GIT. Vasoactive intestinal peptide decreases smooth muscle contractility and increases secretory activity.
Functions of the enteric nervous system
The enteric nervous system is concerned with the gastrointestinal tract and its functions are mainly directed to GIT. The normal functioning of the enteric nervous system is crucial as any abnormality in GIT functioning is distressing and may prove fatal if ignored.
Control of motility
The muscular layer of GIT is responsible for the breakdown of the food and mixing it with the enzymes. It’s also responsible for the forward propulsion of food. The muscles also relax and make available room for the ingested food; this function is most developed in the stomach where ingested material is stored and in the colon where the waste material is stored. The activity of excitatory and inhibitory neurons is coordinated so that appropriate groups of neurons contract and relax in a specific way to propel the intestinal content. Usually, food reaches from mouth to stomach in about 10 seconds by virtue of peristalsis. In the stomach, food is mixed with gastric juice which starts chemical digestion. Stomach contractions also occur to churn the food and mix it thoroughly with the gastric enzymes. The stomach empties food in the duodenum in about 1 to 2 hours. In the small intestine, food is mixed with pancreatic and biliary secretions which further break the food particles into simple absorbable particles, and unabsorbed material is propelled into the large intestine in about 4 hours. Unabsorbed food may stay in the large intestine for 1 or 2 days.
Throughout the GIT, the propulsive action follows a definite pattern. The preceding portion of GIT contracts while the receiving portion relaxes to accommodate the incoming content. In this way, the bolus moves from the oral to the aboral direction. The intrinsic reflexes of the ENS are essential to generate, regulate and control the movement pattern in the small and large intestines.
In the intestines, intrinsic movements are designed for food mixing and propulsion. However, the peristalsis in the stomach isn’t solely due to ENS. Instead, it’s mediated through the interactions of the vagus nerve and the enteric nervous system. When the bolus arrives, the proximal stomach portion relaxes which is brought about by the vagus nerve. Thus, the primary control center for gastric motility is in the brain stem while for the intestines, integrative centers are located in ENS.
Similarly, the peristaltic activity of the esophagus is also controlled by integrative centers in the brainstem. Due to these observations, it’s believed that the enteric nervous system acts as a modifier in the esophagus and stomach while in the intestines it acts as the primary system to generate and regulate motility.
The sphincters in the gut also alter motility. The sphincters relax in response to the reflexes which arise proximal to the sphincter while they contract in response to the reflexes distal to the sphincter and prevent backflow of the contents. The motility of GIT is influenced by the extrinsic sympathetic nervous system which releases adrenaline and decreases the contractility of smooth muscles in GIT.
Local blood blow and fluid exchange regulation
Local blood flow to the GIT mucosa is regulated through the enteric vasodilator neurons to ensure sufficient blood flow for appropriate nutrition and fluid exchange between blood and gut lumen. There are no intrinsic vasoconstrictor neurons in the enteric nervous system. The overall vascular tone of GIT is under the control of extrinsic sympathetic fibers which constrict the vasculature at the time of emergency to divert the blood flow toward vital organs and muscles.
The enteric nervous system regulates the fluid and electrolyte exchange between the blood and gut lumen. This action is mediated through the activity of secretomotor fibers which innervate the mucosa of small and large intestines and alter its permeability. A huge amount of fluids cross the intestinal epithelial surfaces each day. The control of this fluid transport is of prime importance for optimum health. It is controlled by enteric reflexes which are prone to alteration via the extrinsic sympathetic nervous system.
Regulation of gastrointestinal secretions
The enteric nervous system is involved in regulating gastric and pancreatic secretions. It also interacts with the gastrointestinal endocrine cell to modulate their activity. Gastric acid secretion is under the control of both neurons and hormones. Neuronal regulation is mediated through cholinergic fibers which receive excitatory input from vagus or enteric nerves. Pancreatic bicarbonate secretion is controlled by secretin, a hormone released from the duodenum by the synergistic action of cholinergic and noncholinergic enteric neurons.
Defense reactions
The enteric nervous system is involved in defense reactions against pathogens in GIT. In microbial infections, diarrhea ensues to eliminate the offending agent. There is increased fluid secretion in this condition mediated by the enteric secretomotor fibers. However, if the condition doesn’t resolve, fluid loss can lead to hypovolemia and shock.
ENS-CNS interactions
The gastrointestinal tract is under the influence of both ENS and CNS. The afferent neurons transfer signals to the brain about the general condition of GIT. It produces the sensation of pain or irritation in GIT. Moreover, the sense of hunger or satiety is also produced by afferent fibers as well as blood glucose. Other signals such as the number of enzymes in the intestines, and nutrient load in the intestines don’t reach the conscious perception. CNS provides signals to control the GIT response which are mostly relayed through the enteric nervous system.
For example, the sight of food starts preparatory events for digestion in the GIT such as increased salivation and gastric acid secretion. When food is ingested, it stimulates the pharynx and upper esophagus which communicate information to the brain stem and relay information to enteric neurons to increase gastric acid secretion for the arriving food. Similarly, enteric signals from the colon and rectum are relayed to the defecation center in the CNS which sends efferents to enteric neurons to elicit the programmed set of movements to eliminate the unabsorbed material. The defecation reflex can also be inhibited consciously by higher brain centers.
Summary
The enteric nervous system is the network of neurons linked to the gastrointestinal tract and controls the functioning of GIT. It comprises two main neuronal complexes, the myenteric plexus, and Meissner’s plexus.
The myenteric plexus is present between the circular and longitudinal muscle layers of the muscularis externa while Meissner’s plexus is present in the submucosa of GIT. These two plexus are interlinked by numerous connections.
The myenteric plexus controls the coordinated motility of GIT by promoting the contraction and relaxation of specific muscle groups in such a way that the preceding portion of GIT contracts while the succeeding portion relaxes to ensure the movement of contents from mouth to anus.
The submucosal plexus is concerned mainly with the secretion and absorption in the GIT.
The enteric nervous system comprises several neuronal sets including primary afferent neurons, excitatory circular muscles motor neurons, inhibitory circular muscles motor neurons, longitudinal muscle neurons, ascending & descending interneurons, intestinofugal neurons, vasomotor neurons, and secretomotor neurons.
These neuronal sets are interlinked and also form associations with the central nervous system to control the overall functioning of GIT. The primary neurotransmitters in ENS include acetylcholine, serotonin, substance P, enkephalins, endorphins, nitric oxide, and vasoactive intestinal peptides.
In addition to regulating GIT motility and secretions, the enteric nervous system is also involved in defense reactions such as diarrhea, local blood flow regulation in GIT, and several types of ENS-CNS interactions.
References
Tobias A, Sadiq NM. Physiology, Gastrointestinal Nervous Control. [Updated 2022 Sep 26]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2022 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK545268/


